In this newsletter, we return to our exploration of the intestinal tract from a natural health perspective, but this time we shift gears a bit. So far, we’ve covered everything from the mouth through the duodenum (taking time to discuss the ancillary outpouchings along the way: the pancreas, liver, and gallbladder). And throughout, the emphasis has been on digestion. But now as we reach the small intestine, things change. Absorption becomes the dominant issue. Yes, a great deal of digestion still occurs in the small intestine, and we will cover that, but the overall emphasis is on absorption. In fact, if you ignore exceptions like the direct absorption of alcohol from an empty stomach, close to 100% of all nutrient absorption in the human body takes place in the small intestine. Obviously then, its proper functioning is crucial to our health.
In this issue, we will explore the anatomy of the small intestine to give us a functional understanding of how it is constructed to do its job and also provide us with a shared vocabulary that we can subsequently use as we explore exactly how the small intestine completes digestion of food and selectively absorbs the nutrients your body needs.
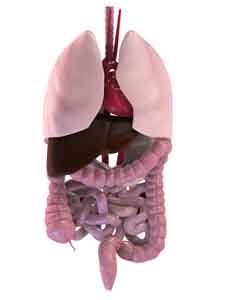
Macro anatomy of the small intestine
The small intestine, also called the small bowel, serves two primary functions in the body.
- If the diet consists primarily of cooked and refined carbohydrates and fats, and if no supplemental enzymes are taken with your meals, these compounds will be mostly intact when they reach the small intestine. Digestive juices in the stomach work on proteins, not carbs and fats. That means that for most people, the small intestine is the final stage for the enzymatic digestion of carbohydrates and fats – keeping in mind that oftentimes they are never fully digested and pass unabsorbed into the bowel where they contribute to gas and bloating as bacteria begin to work on them.
- That said, the primary role of the small intestine is the absorption of nutrients broken down by digestion. These include, the absorption of:
- Proteins (amino acids)
- Carbohydrates (monosaccharides)
- Fats (lipids)
- Vitamins
- Minerals
- Enzymes
- Water
Technically, the small intestine begins at the pylorus valve that separates the stomach from the duodenum and ends at the ileocecal valve that separates the ileum from the large intestine. The bulk of the small intestine is suspended from the body wall by an extension of the peritoneum called the mesentery. The small intestine is approximately 20-23 feet long, depending on how and when it’s measured, and it is divided into three sections:
- Duodenum
- Jejunum
- Ileum
Although precise boundaries between these three segments of bowel are not readily observed, there are microscopic structural differences among them.
Duodenum
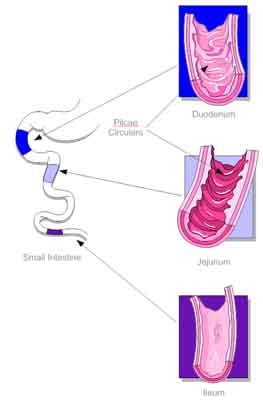 The name duodenum actually derives from its length and literally means “twelve” inches. It runs from the pylorus valve to the ligament of Treitz (a band of smooth muscle that extends to the diaphragm and works to hold the small intestine in place). Although technically part of the small intestine, the duodenum is almost 100% involved in digestion, not absorption. As such, we have discussed it in great detail already and will not focus on it in this newsletter.
The name duodenum actually derives from its length and literally means “twelve” inches. It runs from the pylorus valve to the ligament of Treitz (a band of smooth muscle that extends to the diaphragm and works to hold the small intestine in place). Although technically part of the small intestine, the duodenum is almost 100% involved in digestion, not absorption. As such, we have discussed it in great detail already and will not focus on it in this newsletter.
Jejunum
The jejunum runs from the ligament of Treitz to the mid-small bowel and encompasses roughly 40% of the length of the small intestine. It has numerous muscular folds called plicae circulares, and we will explore it in some detail in the next newsletter. The term “jejunum” derives from the Latin and means “empty of food.” The name, however, actually came from the ancient Greeks who noticed that at death this part of the intestine was always “empty of food.” Hence, the name jejunum.
Ileum
The third division of the small intestine is the ileum, which runs from the mid-small bowel to the ileocecal valve at the entrance to the large bowel (colon) and encompasses roughly 60% of the length of the small intestine. The word “ileum” comes from the ancient Greek and means “twisted,” which actually has a dual meaning. First, when viewed during surgery (or after a Trojan sword has slit open your midsection), the ileum actually looks twisted. The second reference is that the ileum is most often the site of twists that can cause obstructions in the small intestine.
Plicae circulares
As mentioned above, when referencing the jejunum, the small intestine is not flat internally, but is thrown into circular folds. These folds are known as “plicae circulares” and are prominent inside the small intestine from the duodenum to the mid-ileum. They serve a dual purpose:
- They increase surface area for enhanced absorption.
- They cause the chyme to move through the small intestine in a corkscrew motion, which aids in mixing the chyme. Effectively, the folds act as baffles.
Blood supply of the small intestine
Identifying the blood supply of the small intestine is more important for surgeons than for our discussion of the small intestine as it relates to natural health. Nevertheless, very quickly:
- The duodenum is supplied by the gastroduodenal artery and by branches of the superior mesenteric artery.
- The jejunum is supplied by jejunal branches of the superior mesenteric artery.
- The ileum is supplied by the ileal, right colic, ileocolic, and appendiceal branches of the superior mesenteric artery.
The microstructure of the small intestine
If examined closely, the surface of the small intestine has the appearance of soft velvet. This is because it’s covered by millions of small projections called villi which extend about 1 mm into the lumen (the empty space inside the small intestine). But villi are only the most obvious feature of the intestinal wall. As we’ve already discussed, the mucosa (the innermost layer of the intestinal wall) contains a number of different cells including: a self-renewing population of epithelial cells, secretory cells, and endocrine cells. Let’s look at the intestinal wall in a little more detail.
The small intestine has the same four layers as the rest of the GI tract, but they are modified for maximal absorptive power.
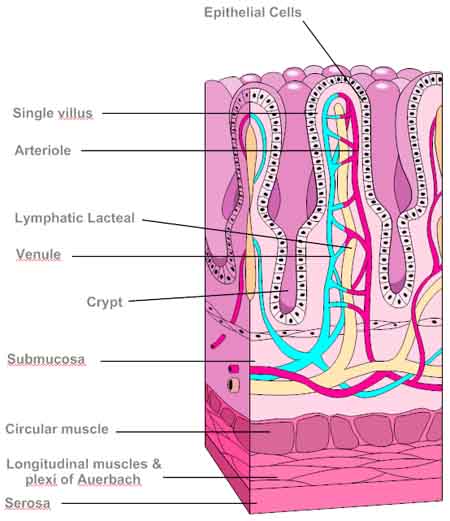
- Serosa — the peritoneal covering of the external surface of the small intestine.
- Muscularis – the muscle layer that governs peristalsis. In particular, it contains:
- A thin layer of longitudinal muscles that stretches the intestine.
- A thicker layer of circular muscles that closes off sections of the intestine as required to allow the intestine to work, move, and grind the chyme in that section over and over before it releases it into the next section of the small intestine…where the process repeats again. We will explore this action in more detail in the next newsletter. (Note: paralytic ileus is the absence of normal GI tract muscle contractions (peristalsis) and can be caused by anything that irritates the peritoneum sufficiently.)
- Myenteric plexi of Auerbach, which coordinate peristalsis. Specifically, the plexi (intersecting groups of nerve cells) are located in the longitudinal muscle layer of the small intestine. The nerve cells in each plexus primarily project to the circular muscle layer and play an important role in regulating gut motility.
- Submucosa – connective tissue. The submucosa consists of dense connective tissue, although fat cells may be present. In fact, all three sections of the small intestine (the duodenum, the jejunum, and the ileum) are all characterized by modifications of the submucosa. The submucosa in the small intestine contains:
- Arterioles, venules, and lymphatic vessels (lacteals) that regulate the flow of blood and lymph fluids going to and from the mucosa of the small intestine. As a side note, the lymphatic vessels also play a key role in the absorption of fats from the small intestine, something we’ll talk more about a bit later.
- Mucosa – villi. This is the grand prize, where most of the action in the small intestine takes place. Accordingly, we will now focus on this layer.
Villi
Villi are projections into the lumen covered predominantly with mature, absorptive enterocytes, along with a spattering of mucus-secreting goblet cells. These cells live only for a few days, die and are shed into the lumen to become part of the chyme where they are digested and absorbed. And yes, if you wish to think of it that way, we are all cannibals eating our own intestinal walls. The word villi literally means “tuft of hair,” which is exactly what the villi look like. In fact, they are fingerlike projections of the mucosa, with approximately 40 villi/sq mm inside the wall of the small intestine. As discussed earlier, each single villus contains an arterial and venus capillary (arteriole and venule) and a lacteal (the lymphatic equivalent of a capillary). Note: the lymphatic system is a circulatory system that exchanges fluid between cells, drains into veins in the neck, and can absorb fat. In the small intestine, the lacteals transport fat from the digestive tract into the circulatory system.
Microstructure of a single villus
Each villus contains multiple absorptive cells on its surface. And protruding from the surface of these absorptive cells on each villus are a vast multitude of microvilli. Microvilli are minutely small hair-like projections that serve to increase the surface area of each villus.
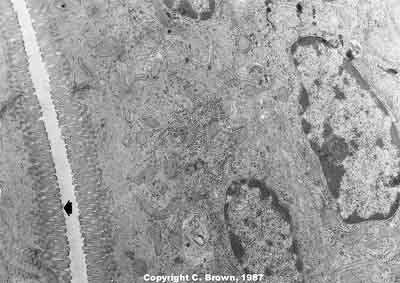
Microvilli lined up along the edge of a villus
How many microvilli are we talking about?
Hold your breath. Each villus has approximately 200 million microvilli/sq mm. This creates a velvety surface on the walls of the small intestine known as the brush border.
And how much does the brush border of microvilli increase the surface area of the wall of the small intestine involved in nutrient absorption?
Again, hold your breath.
All in all, if the small intestine is viewed as a simple pipe, its surface area totals about half a square meter. But it is not a simple pipe. Factor in the mucosal folds, the villi, and the microvilli, and the absorptive surface area of the small intestine is in fact approximately 250 square meters – the size of a tennis court! This increases the absorptive power of the small intestine exponentially.
Intestinal glands are located in the crypts of Lieberkuhn at the base of the villus (see illustration above). The cells/glands here secrete intestinal juices. Toward the base of the crypts are stem cells, which continually divide and provide the source of all the epithelial cells in the crypts and on the villi. The way they divide is actually quite interesting. One daughter cell from each stem cell division is retained as a stem cell – thus perpetuating the untainted original source. The other daughter cell differentiates along one of four pathways to become either an enterocyte, an enteroendocrine cell, a goblet cell, or a Paneth cell. Enterocyte cells migrate up the crypts, and onto the villi, where they become the mature epithelial absorptive cells essential for extracting nutrients from the chyme. Virtually all nutrients, including all amino acids and sugars, enter the body across these absorptive cells that form the epithelium covering the villi.
Note: After crossing the epithelium of the villi, most nutritional molecules diffuse into the capillary network inside the villus diagrammed above, and then into the bloodstream. Some molecules, fats in particular, are transported not into capillaries, but rather into the lymphatic vessels (lacteals), which drain from the intestine and rapidly flow into blood via the thoracic duct.
Specifically, cells/glands found in the crypts of Lieberkuhn, at the base of villi, include:
- Paneth cells are in the deepest part of the glands. They secrete lysozyme (a bacteriocidal enzyme), and they are phagocytes. Their purpose is to protect against invaders that have made their way into the intestinal tract along with the food we eat.
- Enteroendocrine glands are the deepest part of the glands. The cells here secrete three hormones: secretin (S-cells), CCK (CCK-cells), and gastric inhibitory peptide (K-cells).
- Brunner’s glands are in the deepest part of the duodenal mucosa. They secrete alkaline mucous to neutralize acid.
- Goblet cells secrete lubricating mucous.
- Peyer’s patches are sections of lymphatic tissue that detect foreign elements in the GI tract and signal the immune system. (Again, you can bring a lot of bad stuff in through your mouth that needs to be dealt with.)
Ileocecal valve
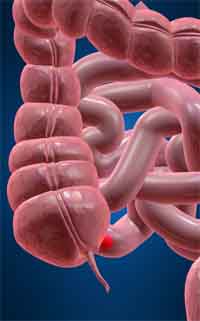 The ileocecal valve is a small muscle located on the right side of the body (left side on most illustrations) between the small and large intestine, thus marking the end of the small intestine. It is essentially a one way check valve that allows the final stage of chyme to pass into the large intestine for final water extraction and stool making. (Note: once chyme enters the large intestine, it is called fecal matter.) If functioning properly, the valve will open and close as required. Unfortunately, it doesn’t always function properly. Sometimes it sticks in the open position, which allows fecal matter to back up into the small intestine, where it can then contaminate the nutrient extraction process. And sometimes the valve sticks in the closed position, which can lead to constipation. Both of these conditions are very toxic and are easily triggered by bad diet (heavy alcohol consumption in particular), dehydration, and stress.
The ileocecal valve is a small muscle located on the right side of the body (left side on most illustrations) between the small and large intestine, thus marking the end of the small intestine. It is essentially a one way check valve that allows the final stage of chyme to pass into the large intestine for final water extraction and stool making. (Note: once chyme enters the large intestine, it is called fecal matter.) If functioning properly, the valve will open and close as required. Unfortunately, it doesn’t always function properly. Sometimes it sticks in the open position, which allows fecal matter to back up into the small intestine, where it can then contaminate the nutrient extraction process. And sometimes the valve sticks in the closed position, which can lead to constipation. Both of these conditions are very toxic and are easily triggered by bad diet (heavy alcohol consumption in particular), dehydration, and stress.
It should be noted that problems with the ileocecal valve are, for the most part, not acknowledged by the medical community, almost never diagnosed, and no effective treatments are offered. Fortunately, there are highly effective natural health options.
Conclusion
In our next issue of the newsletter, we will begin an exploration of exactly how the small intestine (based on its anatomy) does its job — both mechanically and chemically. We will also discuss its physiology, what can go wrong, and how we can fix it…without the need for surgery or debilitating pharmaceutical drugs.











This really helped with my
This really helped with my Biology assignment, many
this website is too long so
this website is too long so it makes it overwhelming. You should have used words that would make this website easier to understand. I barely read because of its “overwhelming” power. I hope you can fix these mistakes…
P.S people do not read thing that look overwhelming…
BYE!! =( BAD WEBSITE
Found the website very useful
Found the website very useful and contained sufficinet information. Have recomended it to others.
i am studying first year mbbs
i am studying first year mbbs . i want to learn more
i write this on behalf of my
i write this on behalf of my wife,just been diagnosed with muscle failure of the small bowell is my understanding,very helpful information thank you!!! now await,/ any possible treatment.
I have found your articles
I have found your articles great and easy to understand even for university study, the diagrams and illustrations WOW Thanks.
Thanks Deanna! It means a
Thanks Deanna! It means a lot.
Excellent article.
Excellent article.
Very informative with understanding our digestive tract.