There’s always plenty of disturbing news coming from the world of pharmaceuticals and mainstream medicine — from the epidemic rates of prescribing errors to the omnipresence of hospital-borne infections. But if Western medicine is riddled with landmines, it is not without its miracles. Take, for instance, the development of fetal surgery.
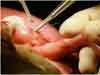
Amazing as it seems, doctors are now able to perform operations before birth on babies who have birth defects.1 To reach the fetus, the attending surgeon actually lifts the uterus almost out of the mother’s body, and then cuts into it. If such gory drama appeals to you, you can watch a You Tube video of a prenatal surgery here. The most common prenatal surgery at this point involves babies with severe spina bifida. Without such surgery, most children with severe spina bifida won’t ever be able to walk and will suffer from profound cognitive impairment. With the surgery, the outlook looks measurably brighter.
Spina bifida means”split spine.”2 It occurs when the spinal cord doesn’t close up completely, allowing leakage of spinal and amniotic fluids. Although about one or two out of every 1000 kids is born with this condition, most have just a mild version that causes little difficulty.3 Some kids, though, have a more severe variation in which leaking fluids create a sac that actually protrudes from the opening in the spine. In these cases, the fluids can build up inside the skull and around the spine, causing paralysis, lack of bladder and bowel control and a condition called hydrocephalus that damages the brain. Kids with hydrocephalus can manifest mental retardation, seizures, and visual impairments.
Treatments for severe spina bifida have historically commenced after birth and have involved surgically closing the hole in the spine and placing a shunt in the brain to reduce fluid build-up. But a recent study published in The New England Journal of Medicine found that babies who went the traditional route, getting operated on after birth, didn’t fare as well as those who received prenatal surgery. The study involved 200 pregnant women, half of whom opted for prenatal surgery. The others had babies who underwent surgery after birth. The children were followed for several years and by the age of three, twice the number of kids who had prenatal surgeries were able to walk normally — 42 percent versus only 21 percent of those who had surgery after birth. Also, four-fifths of the kids who had post-natal surgery needed brain shunts, whereas only half of the kids who had fetal surgery did. And finally, almost all the babies who got the surgery after birth had displaced lower brains, versus only one-third of the kids who had fetal surgery, meaning the fetal surgery survivors were less prone to brain damage.
The prenatal surgery, though, means increased risk for the mother. Also, it ups the chance of premature birth by 79 percent. And, survivors of prenatal surgery still typically suffer from impaired bladder and bowel control, but that’s certainly a trifle compared to serious retardation and paralysis.
Another realm into which prenatal surgery has moved involves removing masses from fetal lungs in order to prevent heart failure upon birth, and also, removing tumors from the tailbone.4 Then there’s laser separation of twins in utero in cases where the blood flow between the twins is abnormal. Lasers also have been used to correct blood vessels connecting the placenta between mother and baby in a frequently fatal condition called Vasa Previa.5 And surgeries have been done to correct urinary blockages in utero, replace damaged lung tissue, correct hernias, and repair heart problems, with varying success. Still, the majority of experts agree that the potential is huge to prevent adult disease by catching it at incipient stages, so plenty of research is going on and the field of fetal surgery is growing.
On a related frontier, researchers hold out big hope for the possibility of preventing genetic diseases with gene and cell therapy before birth. The most promising studies show that transplanting healthy stem cells from a mother into the fetus may correct genetic damage that would result in inherited conditions like sickle-cell anemia, cystic fibrosis, Huntington’s disease, various immune disorders, neurological/muscular conditions, and even diseases like diabetes, hypertension, and certain cancers.
By the way, harking back to spina bifida, it turns out that a healthy lifestyle does play a role in prevention. Studies have shown a strong link between development of the condition and a lack of folic acid. And folic acid abounds in those vegetables we always push here at the Baseline of Health Foundation: the leafy greens, not to mention broccoli, cauliflower, beets, and lentils. The bottom line is that pregnant women, like Popeye, need to eat their spinach. They also should probably take folic acid supplements. (For more on recommended supplements from preconception on up, click here.) In any event, should you or anyone in your circle be pregnant with a fetus that has birth defects, it’s good to know that there are now options dawning on the medical horizon that hold some promise.
1 Knox, Richard.”A Prenatal Surgery for Spina Bifida Comes of Age.” 12 July 2011. NPR. 15 July 2011. http://www.npr.org/2011/07/11/137712436/a-prenatal-surgery-for-spina-bifida-comes-of-age
2“Spina Bifida.” Kids Health. 15 July 2011. http://kidshealth.org/kid/health_problems/bone/spina_bifida.html#
3“Spina Bifida: Topic Overview.” WebMD. 15 July 2011. http://www.webmd.com/parenting/baby/tc/spina-bifida-topic-overview
4“Fetal surgery continues to advance.” 21 February 2010. Science Daily.15 July 2011. http://www.sciencedaily.com/releases/2010/02/100216113859.htmAno
5“Fetal Surgeon Shows For First Time That Laser Procedure May Treat Vasa Previa.” 3 January 2008. Science Daily. <http://www.sciencedaily.com/releases/2007/12/071218101119.htm>